When to Worry About Veins That Appear Out of Nowhere!?
The human vascular system is a complex, high-pressure network of highways that sustain every organ and extremity. Often, we give little thought to the blue or green lines beneath our skin until the moment they suddenly appear to have multiplied or intensified. Discovering prominent veins on your hands, arms, legs, or chest can be a jarring experience, leading many to wonder if their circulatory system is signaling a crisis. While the sudden visibility of veins is frequently a benign byproduct of lifestyle shifts, genetics, or the natural progression of time, understanding the nuances of vascular health is essential for distinguishing a harmless physical trait from a medical warning sign.
To understand why veins appear “out of nowhere,” one must first understand the variables that keep them hidden. Typically, veins are obscured by a combination of skin thickness, dermal elasticity, and a layer of subcutaneous adipose tissue (body fat). When any of these factors are altered, the vascular network is “pushed” to the visual forefront. One of the most common reasons for increased vascularity is a reduction in body fat. When an individual loses weight or undergoes a period of intense physical conditioning, the insulating layer of fat between the muscle and the skin thins out. As this barrier diminishes, the veins have nowhere to go but up against the underside of the skin, creating a more “shredded” or vascular appearance.
Physical exertion itself is a primary driver of temporary and long-term vein visibility. During a workout, especially weight lifting or high-intensity interval training, the body demands an massive surge in oxygenated blood. This increased cardiac output causes the veins to swell as they work to return blood to the heart. Over time, consistent exercise leads to muscle hypertrophy—the growth of muscle fibers. As these muscles expand, they occupy more space beneath the skin, effectively squeezing the veins and forcing them toward the surface. This is why athletes often display prominent vascularity even when at rest; their anatomy has literally been reshaped to accommodate higher blood flow and larger muscle mass.
Environmental factors also play a subtle but significant role in how our veins present on any given day. In hot weather, the body engages in a process called vasodilation. To prevent overheating, the brain signals the blood vessels near the surface of the skin to widen, or dilate. This allows more blood to flow close to the air, facilitating the release of heat and cooling the body down. Consequently, on a humid summer afternoon or after a hot shower, your veins may appear much larger and more blue than they do on a cold winter morning. This is a healthy, self-regulating physiological response, yet it can be surprising to someone who hasn’t noticed the pattern before.
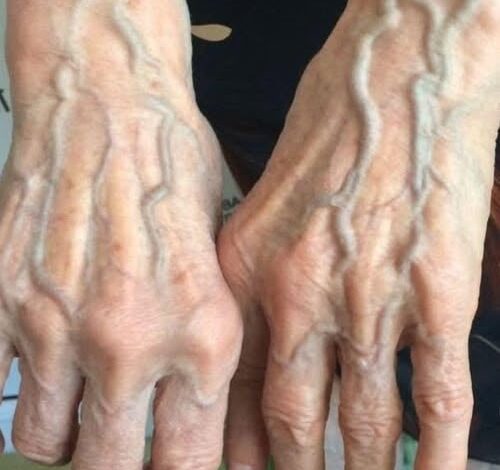
However, the passage of time is the most universal architect of visible veins. As we age, our bodies undergo two inevitable changes: the skin loses its structural proteins—collagen and elastin—and it becomes significantly thinner. This “crepe-like” quality of aging skin lacks the opacity of youth, making the underlying blue and purple hues of the veins much more apparent. Furthermore, the valves within the veins, which are responsible for preventing blood from flowing backward due to gravity, can weaken over time. When these valves struggle, blood can pool slightly, causing the veins to bulge. While this is often a cosmetic concern, it is a primary factor in the development of more pronounced vascular patterns in the elderly.
Hormonal shifts represent another significant, though often temporary, cause for new vascular visibility. Women, in particular, may notice a sudden prominence of veins during pregnancy, menopause, or while undergoing hormone replacement therapy. During pregnancy, the volume of blood in a woman’s body increases by up to 50 percent to support the growing fetus. This massive surge in fluid volume places extra pressure on the veins, often making them visible on the chest, breasts, and legs. Similarly, fluctuations in estrogen and progesterone can affect the elasticity of vessel walls, making them more prone to dilation.
While the aforementioned causes are largely physiological, there are instances where “new” veins demand a clinical evaluation. The primary concern with sudden vascular changes is the development of venous insufficiency or deep vein thrombosis (DVT). You should be particularly vigilant if the appearance of a new vein is accompanied by localized pain, swelling, or a “heavy” sensation in the limb. If a vein appears twisted, rope-like, and dark purple or blue—characteristic of varicose veins—it suggests that the internal valves are failing to move blood efficiently.
More critically, if a vein appears suddenly and is accompanied by redness, warmth to the touch, or significant swelling in just one leg or arm, it could indicate a blood clot. In such cases, the “visible vein” isn’t just an aesthetic shift; it is a symptom of an obstructed pathway. Furthermore, if you notice a “spiderweb” pattern of tiny veins on the chest or face that was never there before, it can sometimes be an external indicator of internal pressure issues or, in certain contexts, liver health concerns.
Maintaining vascular health involves a proactive approach to circulation. Regular movement is the most effective way to keep veins “hidden” and healthy. The calf muscles, in particular, act as a second heart for the body, pumping blood upward against gravity during walking or running. Staying hydrated is equally vital, as dehydration can cause the blood to thicken and the veins to contract, sometimes making them look more prominent and dark. For those who spend long hours standing or sitting, compression therapy can provide the external support necessary to keep blood moving and prevent the pooling that leads to visible bulging.
In the vast majority of cases, a new vein on the back of the hand or along the bicep is simply a sign of a life being lived—a body that is aging, exercising, or adapting to the heat. It is a testament to the incredible, tireless work of the circulatory system. However, the body is an intuitive communicator. By paying attention to the context of these changes—noting if they are accompanied by discomfort or inflammation—you can ensure that your vascular health remains as robust as the network of veins that keeps you moving.