One month before a heart attack – Your body will alert you – Here are 5 symptoms!
The human heart is a marvel of biological engineering, an indefatigable pump that moves thousands of liters of blood through the body every single day. Yet, for all its strength, the heart is also a sensitive instrument, and when it begins to falter, it rarely does so without warning. While the popular imagination often depicts a heart attack as a sudden, thunderous event—the “Hollywood Heart Attack” where a victim clutches their chest and collapses—the medical reality is frequently much more subtle. For many individuals, the body begins broadcasting distress signals as early as thirty days before a major cardiac event occurs. These physiological whispers, if recognized and acted upon, can be the difference between a preventable emergency and a life-altering tragedy.
Understanding the early symptoms of heart failure and impending myocardial infarction requires a shift in how we perceive physical discomfort. We are often conditioned to “push through” fatigue or dismiss minor swelling as a consequence of a long day on our feet. However, in the context of cardiovascular health, these seemingly benign changes are often the early tremors before a seismic shift. By identifying five specific warning signs—edema, chronic fatigue, respiratory distress, systemic weakness, and neurological interruptions—individuals can take proactive control of their heart health long before the situation becomes critical.
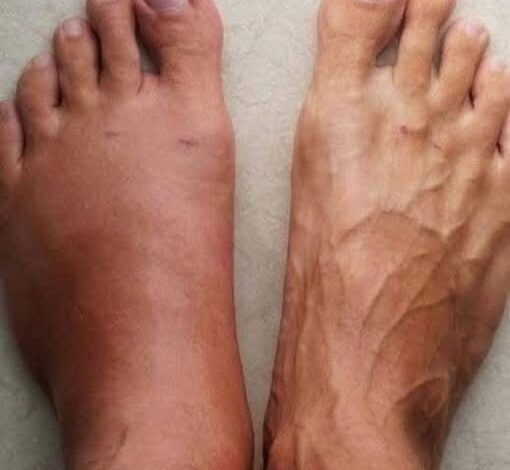
The first and perhaps most visible indicator of a heart under strain is the accumulation of fluid in the lower extremities, a condition known as peripheral edema. When the heart’s pumping action becomes inefficient, as is the case in congestive heart failure, the blood returning to the heart through the veins backs up. This increased pressure in the blood vessels forces fluid into the surrounding tissues, most notably in the feet, ankles, and legs. If you notice that your socks are leaving deep indentations in your skin or that your shoes feel uncharacteristically tight by the end of the afternoon, it is not merely a sign of gravity at work. It is a sign that your heart is struggling to maintain the delicate balance of fluid dynamics within your circulatory system.
A second, and often more insidious, symptom is the onset of persistent, unexplained fatigue and a pervasive sense of drowsiness. This is not the typical tiredness that follows a poor night’s sleep or a stressful week at work; rather, it is a profound exhaustion that persists even after rest. This occurs because narrowed or clogged arteries—the hallmark of coronary artery disease—restrict the flow of oxygenated blood to the heart muscle itself. To compensate for this reduced fuel supply, the heart must work significantly harder to meet the body’s demands. This constant overexertion drains the body’s energy reserves, leaving the individual feeling perpetually drained. When the heart is “starved” for oxygen, the entire body feels the deficit, resulting in a lethargy that can appear weeks before a clinical event.
The third critical warning sign is shortness of breath, or dyspnea, which highlights the inseparable link between the cardiac and respiratory systems. As the heart’s left ventricle weakens, it fails to pump blood out to the rest of the body as effectively as it should. This causes a “backup” of pressure that extends into the pulmonary veins, the vessels that carry blood from the lungs to the heart. This pressure can cause fluid to leak into the air sacs of the lungs, making it increasingly difficult to breathe. You might notice this initially during physical exertion—such as climbing a flight of stairs—but as the condition progresses, it can occur even while resting or lying flat in bed. Breathlessness is the body’s urgent cry for oxygen, and it should never be ignored as a mere sign of being “out of shape.”
Systemic weakness throughout the body serves as the fourth red flag. This generalized frailty is the direct result of poor systemic circulation. When the heart cannot push blood to the furthest reaches of the anatomy, the muscles are deprived of the glucose and oxygen they need to function. This can manifest as a sudden instability, a lack of grip strength, or even unexpected falls. Many patients who later suffer a heart attack recall feeling “heavy” or “clumsy” in the weeks leading up to the event. This physical instability is a clear indication that the peripheral tissues are being rationed by a cardiovascular system that is in survival mode, prioritizing the brain and internal organs over the skeletal muscles.
Finally, the fifth and perhaps most alarming set of symptoms includes sudden dizziness, lightheadedness, and cold sweats. These neurological and autonomic responses occur when the blood flow to the brain is dangerously restricted. If the heart’s output drops below a certain threshold, the brain—the most oxygen-hungry organ in the body—begins to malfunction. Dizziness can be accompanied by a “clammy” sensation or a cold sweat that arises without any physical exertion or heat. This is often a sign of an impending blockage or a dangerous heart rhythm, signaling that the window for preventive intervention is closing rapidly.
Recognizing these five symptoms—swelling, fatigue, breathlessness, weakness, and dizziness—is the first step toward safeguarding your long-term health. The human body is remarkably communicative, but its language is often one of gradual change rather than sudden shouting. A month before a heart attack, the body is already attempting to save itself by sending these alerts. The tragedy lies in the fact that many people rationalize these signs away, attributing them to aging, stress, or minor illnesses.
Taking a “wait and see” approach with cardiac symptoms is a gamble with incredibly high stakes. Modern medicine has an array of tools—from advanced imaging and blood tests to minimally invasive interventions—that can stabilize a failing heart if caught early. Consulting a healthcare provider the moment these patterns emerge allows for a clinical evaluation that can identify narrowed arteries or valve issues before they lead to a full-blown myocardial infarction. In the realm of heart health, knowledge is not just power; it is protection. By paying attention to the subtle shifts in your physical state and respecting the signals your heart is sending, you can rewrite your medical future and ensure that your heart continues to beat strongly for years to come.